Payers
Overview
Payers represent the insurance entities responsible for processing healthcare claims. Businesses can manage these connections, configure covered services, and handle required enrollments for electronic submission and eligibility verification.
Permissions: Payer management and enrollment requests are only available to Business (Team) owners.
Table of Contents
Where to Find It
The Payer management interface is found under Billing → Claims → Dashboard. This area serves as the center for all insurance-related settings for the business.
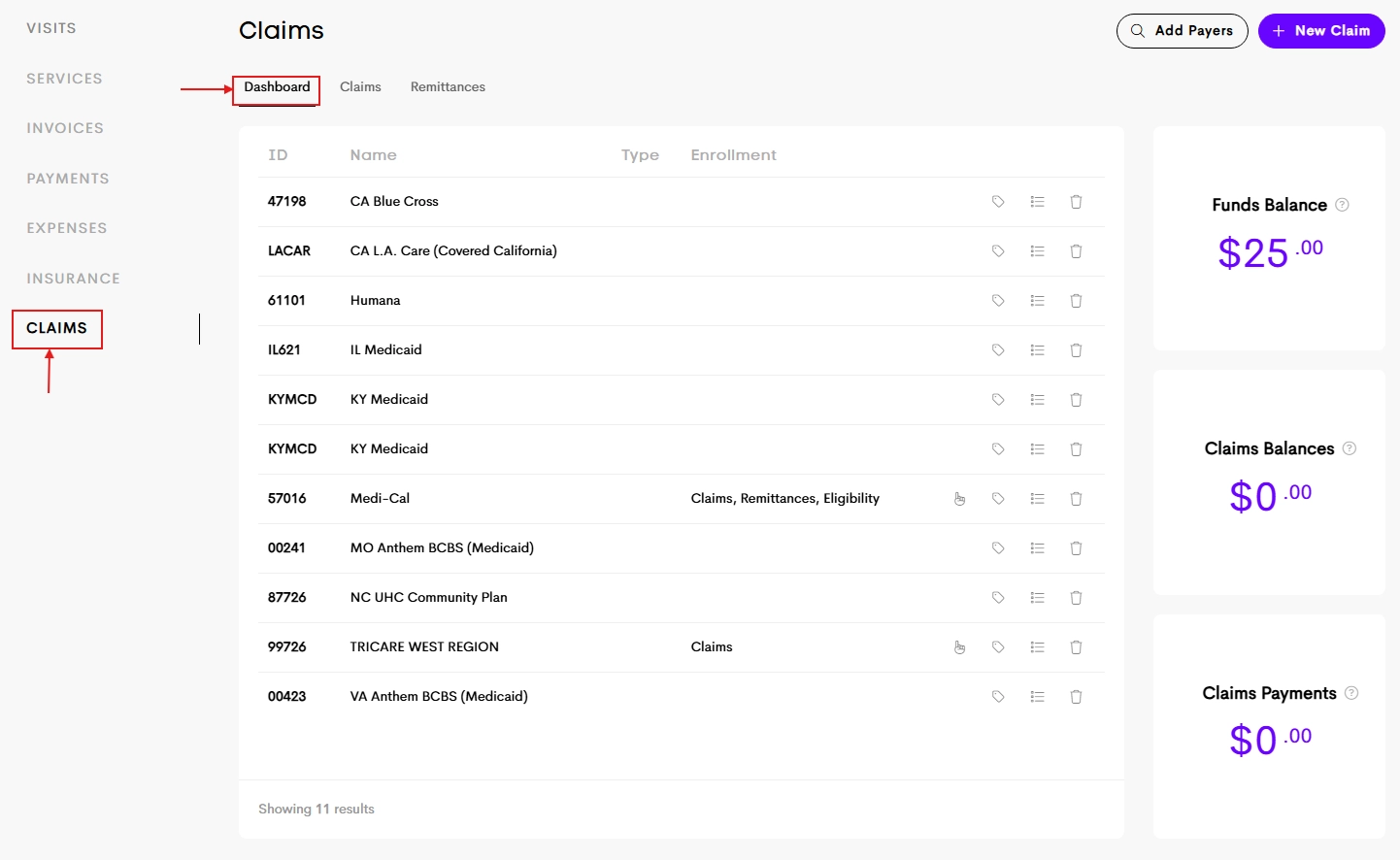
The dashboard displays all payers that you have imported in a table format with the following columns:
- ID: The payer's identifier. This may be the same for multiple payers.
- Name: The full name of the insurance company or payer.
- Type: Badge indicating the payer type (Medicaid vs Commercial). The type only matters for eligibility verifications
- Enrollment: Lists the enrollment types required for this payer (if applicable)
- Related Article: What is Enrollment?
