Claims: Claims + Insurance
When creating a new claim, selecting a payer for a client having an existing insurance record for the payer. The claim pre-fills with the plan and subscriber details to ensure billing consistency and reduce chances of claim rejections.
Additional Criteria To Auto-Populate
Active Coverage: All service dates added to the claim must fall within the plan’s Effective and Expiration dates.
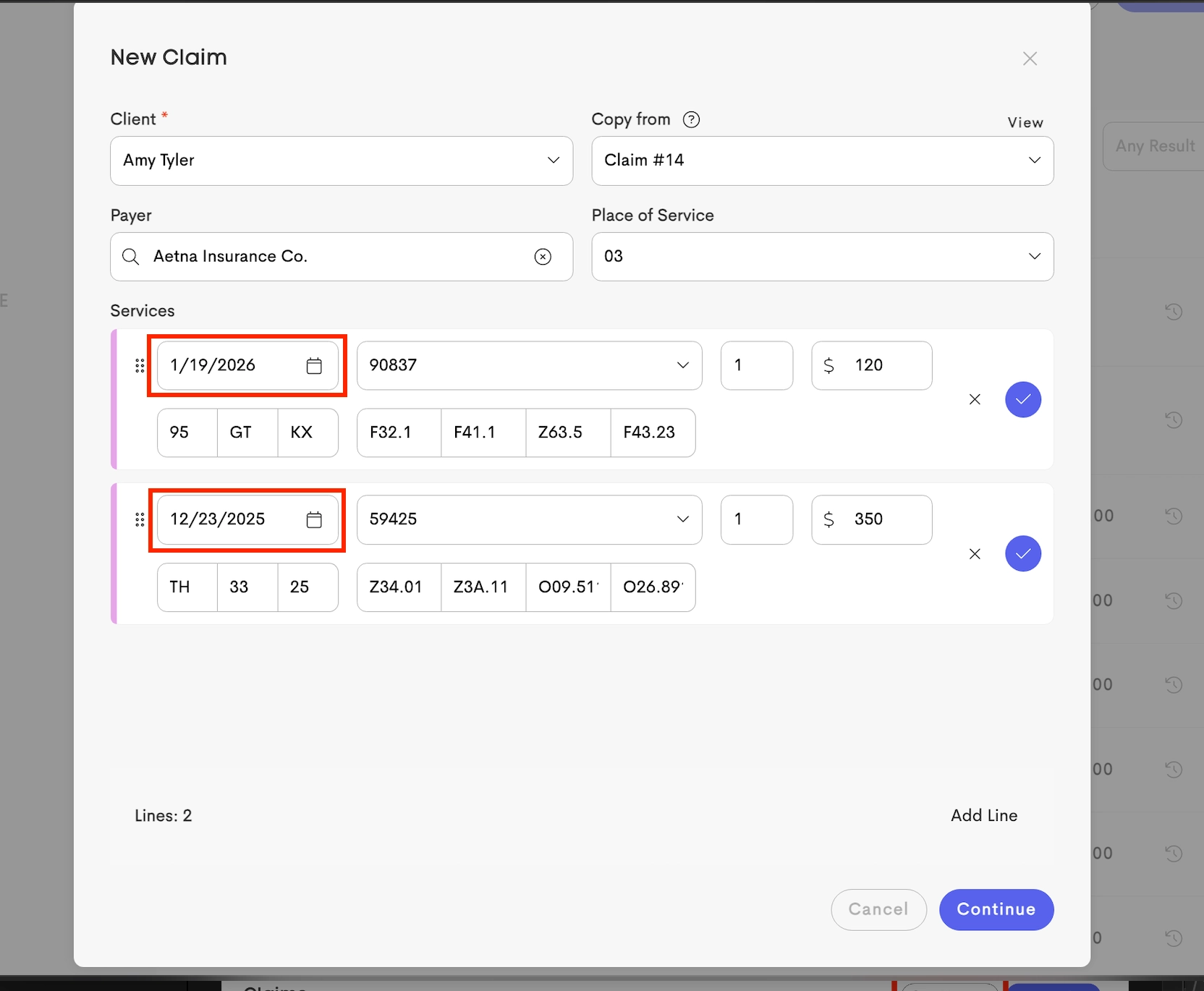
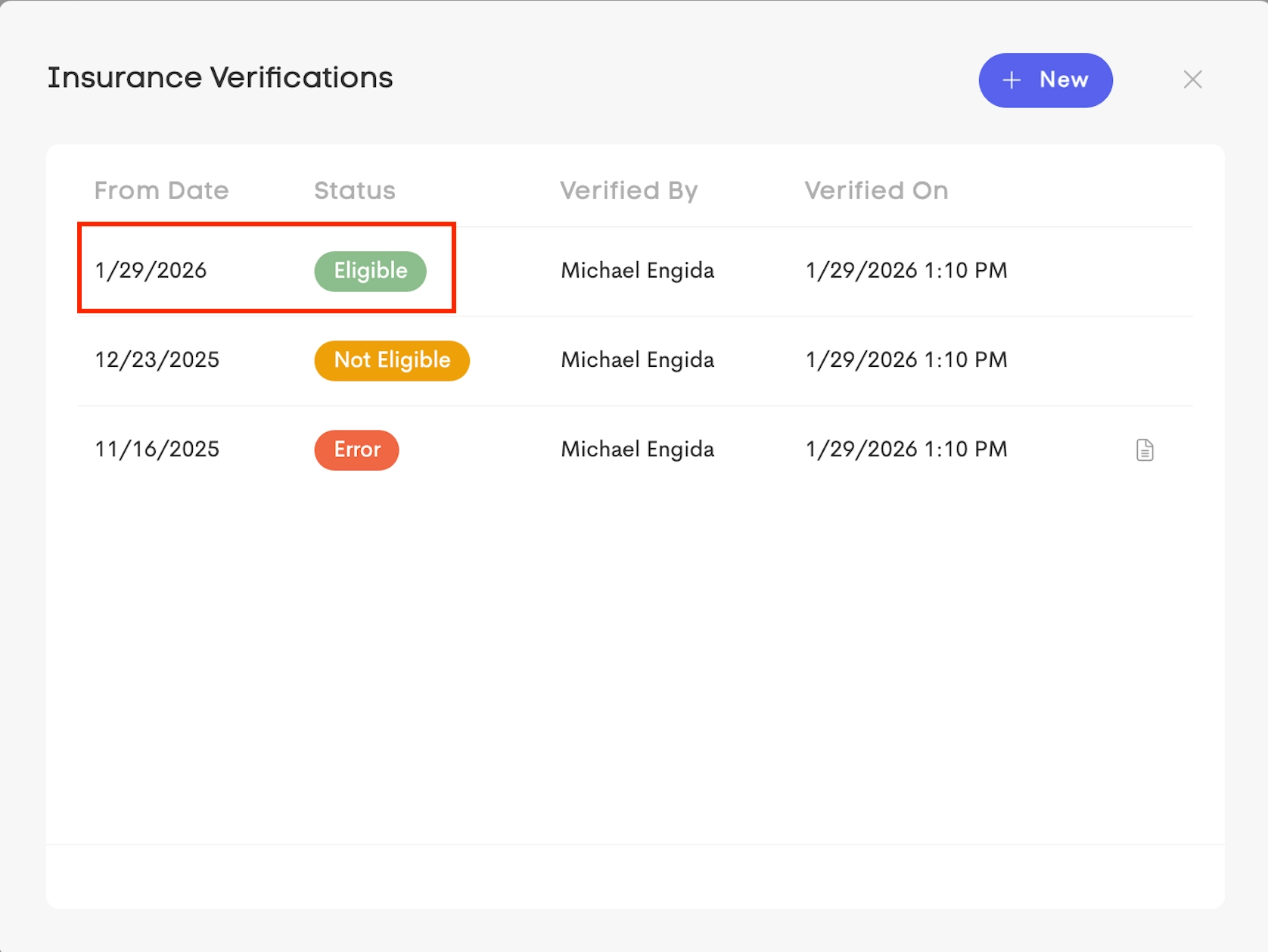
Eligibility Check: The latest verification for that plan must have a status of 🟢 Eligible.
The valid eligibility check must have been performed on or before the earliest service date on the claim.
Field Mapping

|
Box |
Field Name |
Data Source |
|
1a |
Insured's ID Number | Member ID from the Insurance record. |
|
4 |
Insured's Name | First & Last Name of the Primary Subscriber. |
|
6 |
Patient Relationship | The selected Relationship to the subscriber. |
|
7 |
Insured's Address | Full address, city, state, zip, and phone of the primary subscriber. |
|
11 |
Insured's Policy Group | The Group / Program Number. |
|
11a |
Insured's Demographics | Date of Birth and Sex of the primary subscriber. |
|
11c |
Insured's Plan Name | The Plan Name. |
|
13 |
Insured's Signature | Subscriber's First and Last name |
